How an Employer Increased Behavioral Health Engagement at Premise Health by 1,300%
15 years ago, an employer in the financial services industry began a partnership with Premise Health by opening its first health center in Richmond, Virginia.
The client’s commitment to quality healthcare now spans from Virginia to Texas to Nevada. In total, these health centers serve tens of thousands of associates and their immediate family members, including spouses/domestic partners and dependents not enrolled in the client’s medical plan. Members have access to primary care, chronic condition management, physical therapy, nutrition care, pharmacy, and after the conclusion of a successful pilot, behavioral health counseling.

The Challenge
The employer cares deeply for its associates and their family members and strives to help them live healthier lives. After seeing an uptick in leave requests driven by behavioral health needs, the company took action, digging deeper with Premise and its other health and wellness partners to identify the following related trends:
-
- A large percentage of primary care health center visits with behavioral health diagnoses
- A high number of referrals to the employee assistance program (EAP) and other community-based behavioral health providers
- A high percentage of community claims for behavioral healthcare
- A high percentage of pharmacy claims for mental health medications
The Solution
To help address these trends, the client proactively added a counselor at one of its health centers as a pilot. Access to counseling services in the community was a challenge and Premise believed adding onsite counseling services was a natural extension of its pre-existing primary care model. The addition of an onsite counselor would encourage associates to proactively seek behavioral health care, which could likely decrease the number or duration of leave of absences and lead to happier, healthier associates.
The client and Premise collaboratively decided to offer short-term behavioral health counseling to complement their existing benefit strategy, which focuses on job-related and personal coping strategies to address common drivers of stress, anxiety, depression, and attention-deficit/hyperactivity disorder. Compared to traditional counseling, which can be long-term in nature, short-term counseling is time-limited, with an intense, relatively short length of treatment. When working with associates, the counselor taught different lifestyle strategies to help members work through and cope with their stressors, while also encouraging participation in other mental wellness collaborations at the employer’s health centers as a preventive strategy. These efforts not only improved associates’ mental health, but their overall health as well.
The Outcome
By the end of the pilot, the client was encouraged by the promising results it saw. The support provided by the counselor and entire care team helped associates improve their mental and physical health outlook, enabling them to stay at work in many instances. The pilot also overwhelmingly demonstrated how important coordination of care is, with at least 20 behavioral health cases involving interdisciplinary treatment between two or more healthcare disciplines. The overwhelming qualitative success of the pilot led the employer to commit to a full behavioral health expansion at many of their sites across the country.
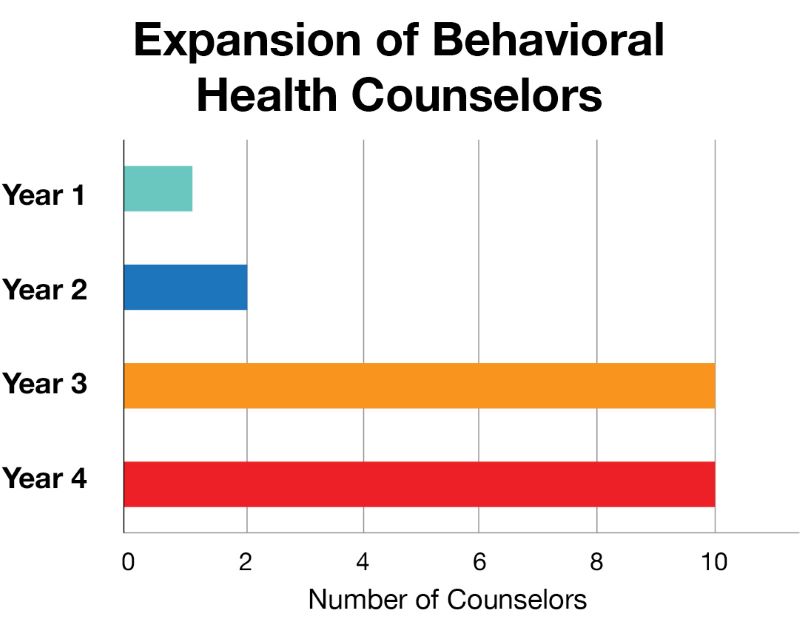
Three years after the pilot, behavioral health is still in high demand for the employer, seeing a 1,300% increase in unique members since the program began. Behavioral health counselors have stayed busy, treating over 2,000 unique members through over 9,000 visits, both in-person and virtually. From concept to pilot phase and now full implementation, the addition of behavioral health counseling was driven by the client’s commitment to the wellbeing of its associates, and Premise is proud to support their efforts.
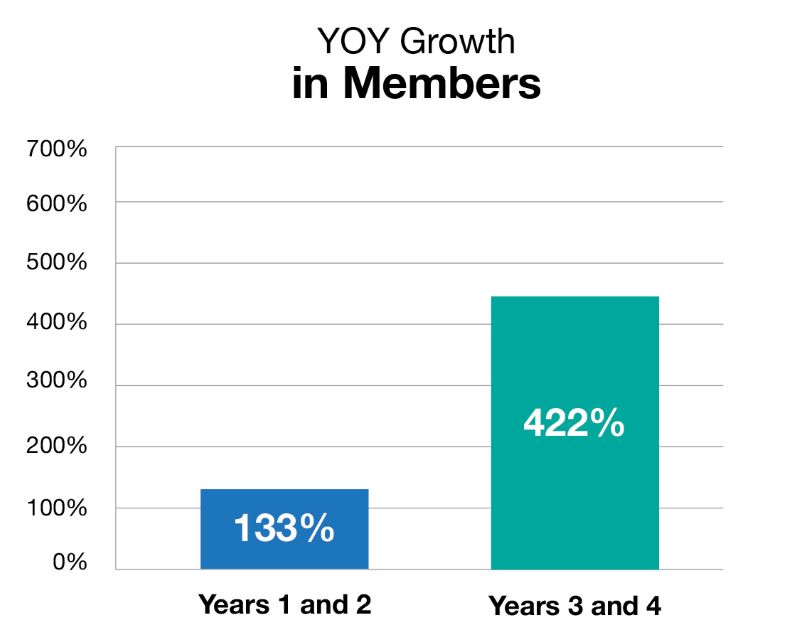
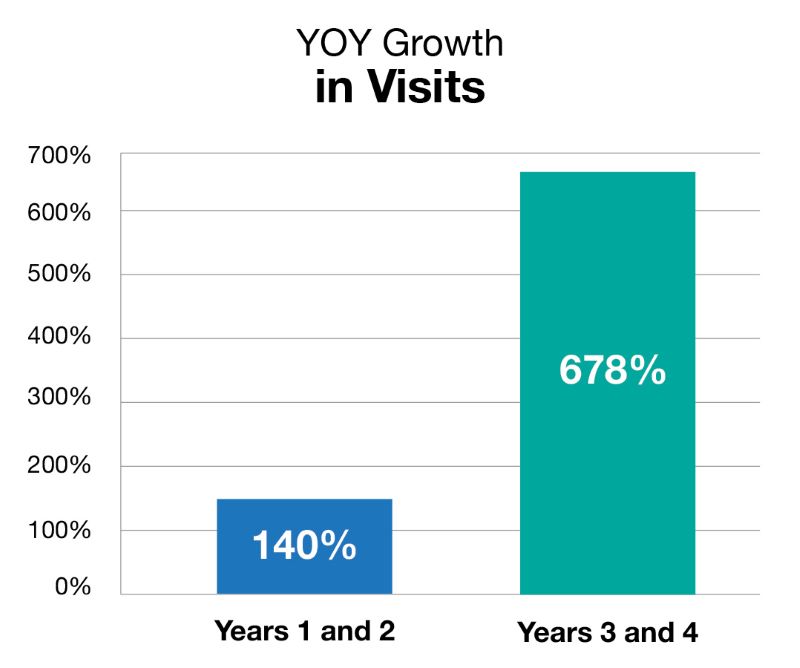
The evaluation period of this study took place over four years from 2018 to 2021.


