How a variable copay program can fully offset a pharmacy’s operating expense
Like many other U.S. employers, our client dealt with rising pharmacy costs tied to expensive medications and increasing chronic conditions among their employee population. This west coast employer partnered with Premise Health to implement a Variable Copay Program aimed at reducing plan costs and offsetting member copays for expensive medications.
The Challenge
In March of 2018, Premise Health rolled out the Variable Copay Program. The program leverages existing assistance programs to reduce plan costs and offset copays for expensive medications. Not only does it help plans save on high cost medications by capturing the maximum benefit of manufacturer copay cards, it also reduces or eliminates member’s copayment responsibility required by the assistance program or original plan design.
While medication therapy works for most chronic conditions, their inflated cost requires complicated financial planning. As a result, navigating high cost therapies are employers number one concern when managing pharmacy benefits1. Compounding this is the fact that the U.S. pays roughly four times more than other countries for the same medications2. Many self- insured employers, such as our client, take on much of the cost.
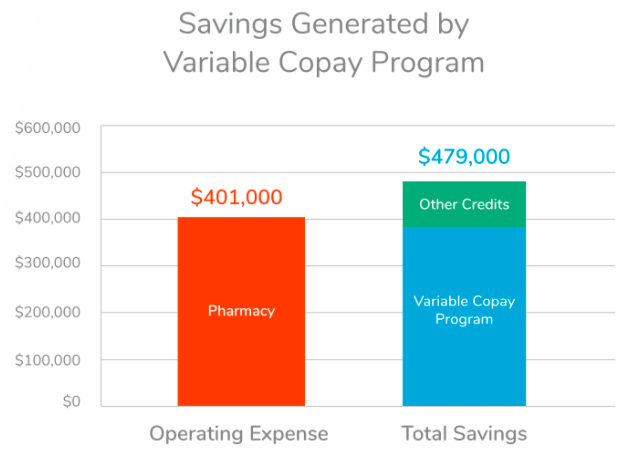
Over the course of a year, the program proved to be a definitive success that ultimately led to 100% member satisfaction and a complete offset of the pharmacy’s operating expense.
- $585 average savings per prescription
- ~$78k savings surplus above operating expense
- 32% of medication costs shifted to copay assistance cards
The Solution
To fully maximize the copay assistance card value, Premise identified medications driving the most pharmacy spend and worked with our client to optimize their benefit plan design and copay structure. The onsite pharmacy staff then proactively identified and enrolled members, guiding them through any necessary copay assistance card requirements.
Copay assistance cards are in essence a coupon; they are funds allocated, implemented and managed by the drug manufacturer to offset member copays for expensive medications.
Our value-based healthcare model focuses on developing personal relationships with members. These relationships, paired with convenient access, make it seamless for pharmacy staff to facilitate the variable copay program while ensuring appropriate care, medication management and treatment adherence. Unlike PBMs, Premise operates outside of the pharmaceutical contracting world making delivering value and savings for clients and members our number one priority.
The Outcome
Over the course of the 2019 calendar year, not only did the program prove to be a resounding success for members and staff, it entirely offset the operating expense of the pharmacy – not to mention a savings surplus of approximately $78,000 over operating costs. Contributing to this were achieved average wholesale price discounts of 42% on specialty medications and 48% on diabetic medications for those that were attributed to the Variable Copay Program.
By capturing the maximum benefit of drug manufacturer copay card values, Premise Health saved our client and members thousands on expensive medications. And thanks to the hands-on approach by Premise pharmacists, enrolled members stayed more adherent to their medications and responded resoundingly positive when surveyed about their experience.
Medication adherence reduces downstream medical costs3
In this study, enrolled diabetic members were more adherent to their medications:
Program Member…………………….85%
State Average…………………………..64%
1. National Business Group on Health, 2020 Large Employers’ Health Care Strategy and Plan Design Survey, 2019, https://www.businessgrouphealth.org/benchmarking/survey-reports/2020-report/
2. Ways and Means Committee Staff, A Painful Pill to Swallow: U.S. vs. International Prescription Drug Prices, September 2019, https://waysandmeans.house.gov/sites/democrats.waysandmeans.house.gov/files/documents/U.S.%20vs.%20International%20Prescription%20Drug%20Prices_0.pdf
3. CVS Caremark State of the State Adherence Report, 2013, http://www.cvshealth.com/sites/default/files/SOS-Adherence-Report-2013_Final_2.pdf


