Employers save $10,693 PMPY when high-risk members use care management and primary care
With six in 10 American adults living with at least one chronic condition1 and organizations now paying billions per year in higher medical costs2, employers can’t afford not to offer personalized support for their high-cost, high-risk members.
The Findings
Our analysis uncovered improved cost savings, member health outcomes, and routine care utilization for organizations that offered care management alongside Premise Health primary care. This supports the idea that organizations who offer integrated chronic condition support as part of an advanced primary care model save on healthcare spend and have a healthier, more engaged population.




Cost Savings
For at-risk populations living with chronic conditions, healthcare costs are significantly higher for both employers and the members they cover. Our analysis found that when these members have the support of care management in addition to primary care services, organizations saw measurable savings, especially for the high-risk members among their population:
>
>
>
Savings with the Premise Health Model
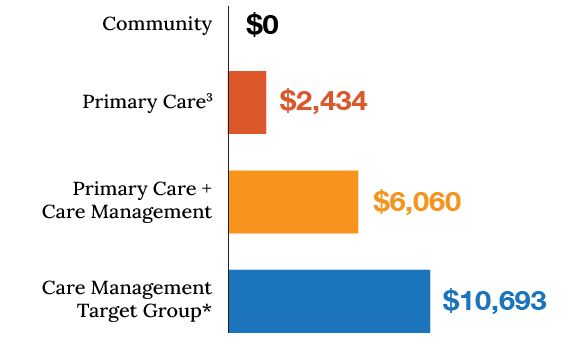
*High-risk members are those whose risk level is in the top 30% of the population. This is often linked to having multiple chronic conditions, but other factors can also contribute to their risk for cost.
Health Outcomes
DIABETES
For members living with diabetes, keeping blood sugar (HbA1c) and blood pressure at healthy levels is a key metric in tracking proper management of the condition. With the support of a care manager, members studied in this analysis experienced more stable health over time:
95% of members had a completed HbA1c screening, which was 10% higher than the community benchmark
82% of members had a blood pressure of less than 140/90 mmHg4, which was 55% higher than the community benchmark and 9% higher than the HEDIS goal value
OBESITY
In addition to tracking changes in average body weight, body mass index (BMI) is also tracked for members meeting medical criteria as overweight and obese, which is the measure of weight relative to height. Members participating in care management saw improvements in BMI and overall weight loss:
On average, members saw a 1.08-point BMI decrease and weight loss of 7 pounds
Those in the top 25% of positive health outcomes saw even better results with an average BMI decrease of 3 points and weight loss of 18 pounds

Primary Care Utilization
Members with uncontrolled chronic conditions often go to the emergency room or urgent care for avoidable health events. For example: hyperlipidemia raises the risk of heart attack, stroke, and other cardiovascular issues, but with early intervention and preventive care, members can manage these risks before they escalate into emergency situations. With the help of care managers, members attributed to Premise were able to stay out of the emergency room because they utilized more preventive primary care services:
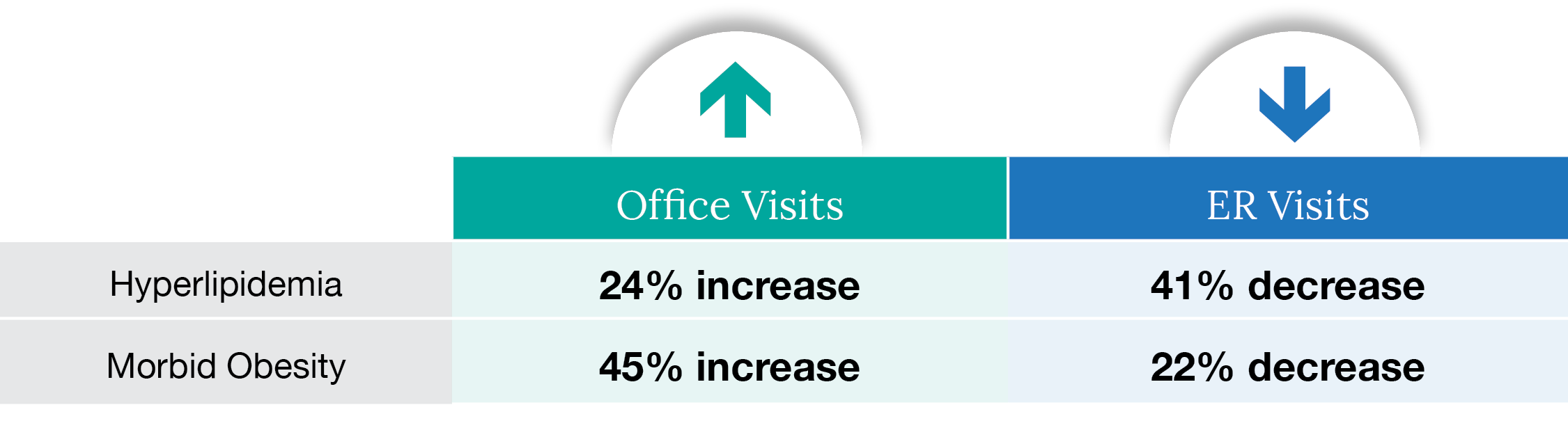
![]()
Routine Screening Utilization
Routine screenings and follow-up care are critically important, especially for members managing complex conditions. Through the guidance of care managers, Premise-attributed members were more adherent to recommended preventive care guidelines when compared to the benchmark:


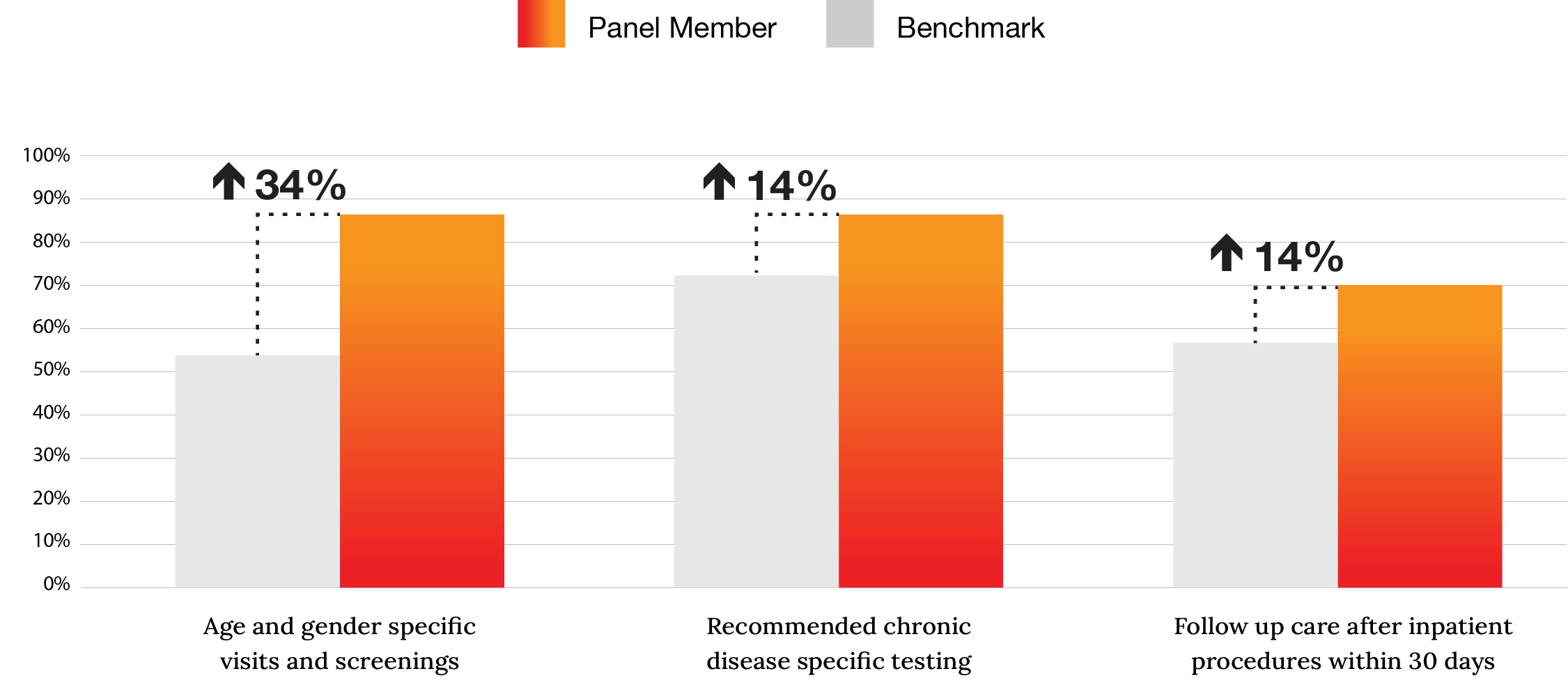
![]()
The Methodology
This study was conducted using 2023 data and analyzed two distinct groups: members attributed to primary care through care management at Premise, and those attributed to Premise primary care without care management. Both groups were compared to their community-attributed counterparts to calculate savings on a per member per year basis, while also accounting for concurrent risks using Milliman advanced risk adjusters, as well as additional factors for care management.
For the purposes of this study, Premise attribution was defined as engaged members that have most of their visits with a Premise provider rather than with community providers. The community refers to any healthcare provider outside of the Premise ecosystem, including private practices, hospital systems, and more. This study compared members in care management on the best available like-for-like basis to members managed by community providers. Using a one-to-many cohort analysis, a comparison cohort was created to match panel members to community-attributed members with a similar distribution of chronic condition mix, age, location, and gender.
The Study
Premise conducted an analysis on our care management book of business which looks at 2023 data of 2,181 unique lives across 13 clients in a variety of industries and geographic regions. The analysis aimed to calculate the reduction in total cost of care clients save when partnering with Premise for care management, including the savings achieved when care management is paired with primary care services. It also examined the cost and prevalence of chronic conditions, the savings associated with those individual conditions, and the compounded savings realized when addressing multiple chronic conditions simultaneously.
Industries Represented
>
>
>
>
>
>
- Centers for Disease Control and Prevention. (2024). About chronic diseases. U.S. Department of Health and Human Services.
https://www.cdc.gov/chronic-disease/about/index.html - GlobalData. (2024). Overweight & obesity: Impact on employers.
https://www.globaldata.com/health-economics/US/Employers/Overweight-Obesity-Impact-on-Employers.pdf - Number reflects average Premise-attributed member savings and contains influence of other products
- Blood pressure of less than 140/90 mmHg in the last 12 months meets recommended HEDIS metrics on managing blood pressure level
https://wpcdn.ncqa.org/www-prod/wp-content/uploads/HEDIS-MY-2024-Measure-Description.pdf


